

Data Analytics is the process of examining data to get insights from, and conclusions about, the information they contain. Increasingly, this requires the aid of specialized systems and software. We design data analytics tools that are widely used in commercial industries to examine the data on a real-time basis and help in the informed decision-making process.
Our applications increase the availability of data to users and secure the data. They help with data analysis and inspection. Data analytics considers your preferences, your needs, locations, and purchase history in the Site Action Menu.
Data visualizations, such as graphs or charts, provide information about the performance of organizations. The human brain processes visual elements more quickly than texts or columns of numbers. Using data analytics, we design a dashboard system that provides graphical representation which is easy to understand without the need for any training.
For a large healthcare organization, the amount of clinical and administrative data constantly rolling in can be staggering. A robust data analytics infrastructure is essential for delivering actionable insights to providers and staff, but the process of balancing scale and usability can be difficult to manage.
As healthcare technology company, we manage a platform that aggregates and normalizes clinical data. This lets organizations use information from any certified EHR in other applications.
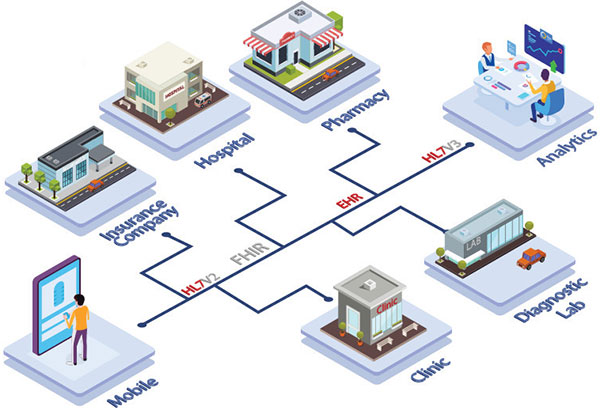
The platform ingests HL7 data from different providers and in different formats. Then it maps into other formats for use downstream.
The foundation of 'data analytics' is the data itself. As they say, 'garbage in, garbage out'. If you're struggling to reconcile and analyze information from many sources, we can help.
You can pull HL7 data sources into business intelligence tools or Excel.
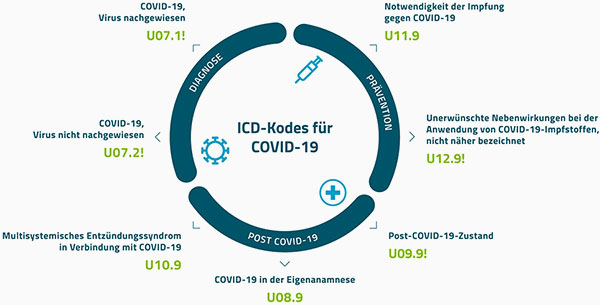
ICD-10 dramatically increases the volume, variety, and specificity of healthcare data. Whereas before much of the detail about a patient’s condition, regimen of care, and outcome of that care was masked by general or unspecified codes, these elements and insights are now standardized and clarified on claims.
ICD-10’s specificity has made claims an even richer source of data. This change brings with it certain challenges—specifically, managing and extracting actionable information from increasingly massive data sets.
Why are some patients readmitted—but not others? That’s a trick question, because how can a researcher ever know why patients readmit if they aren’t even sure (at the data level) what conditions people are really suffering from?
Now with the additional granularity of ICD-10 and the data-mining capabilities to uncover and correlate other data points such as care history, demographic information, and comorbid conditions, researchers and analysts can better see what’s really driving readmissions because they can better “see” the patient in the data.
How do you calculate your claims denials rate? What is your payer mix? Can you benchmark payers based on denials? Do you know what procedures drive the most denials? What procedures do your top payers deny most often?
Much more than a pretty interface, our new dashboards transform your EDI information into organized insights. We map your data to build a single, normalized data set. This data is organized in an intuitive interface that offers you a new level of oversight of the revenue cycle.
